
Our members
You can count on us to ensure our members get the most from their Medicaid plans. Everyone has unique health needs, which is why we offer a wide range of plans for:
- Pregnant mothers and their babies
- Children up to age 19, including foster and adoptive children
- Adults and children living with disabilities or other serious health conditions
- People who need help to live independently
- Seniors who qualify for both Medicare and Medicaid
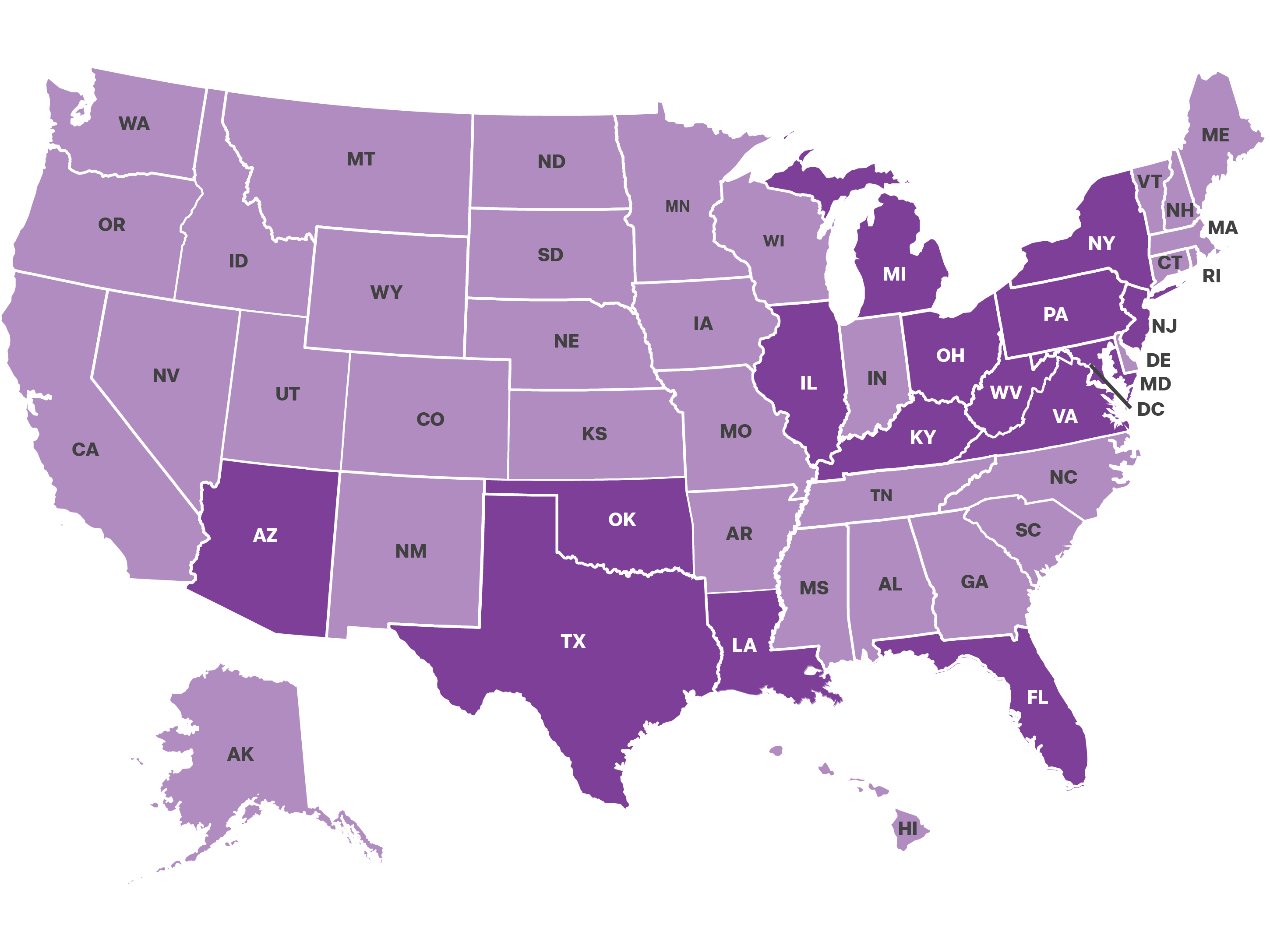
Go to your state’s health plan and see offerings in your state.
National experience, local impact
Aetna Better Health® is proud to be part of the CVS Health® family. Our goal is to be a trusted health partner in the local communities we serve. We take a whole-person approach to Medicaid, bringing together what matters most to health. Through expert care and easier access to services and support, we help our members live their healthiest lives. Because healthier happens together®.
Legal notices
Aetna is part of the CVS Health® family of companies.
